Accelerating Payer-to-Payer Data Exchange for Continuity of Care
PilotFish Enables Payers to Meet CMS Interoperability Requirements for Payer-to-Payer API Exchange
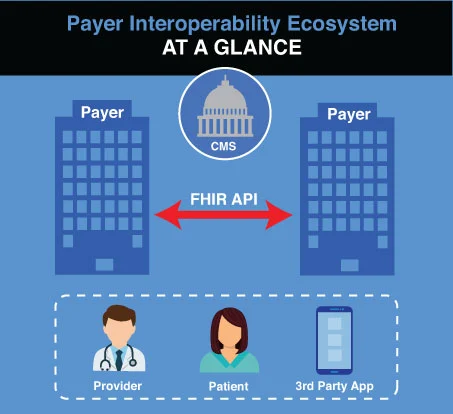
Understanding the CMS Payer-to-Payer API Exchange Requirement
The Centers for Medicare & Medicaid Services (CMS) introduced the Payer-to-Payer API Exchange mandate as part of its broader Interoperability and Patient Access Rule. This regulation requires health insurance payers to implement secure, standards-based API data exchange capabilities that allow members’ clinical information to follow them as they change health plans.
Under the CMS rule, payers must share a member’s complete healthcare record using Fast Healthcare Interoperability Resources (FHIR) APIs. This includes claims data, encounter information, clinical data and demographic details that are essential for care coordination and member safety. By enabling this seamless payer data exchange, the rule ensures that a patient’s health history is always available to their current and future providers.
The CMS Payer-to-Payer Interoperability requirement is designed to achieve three major goals:
- Ensure continuity of care: Members’ clinical and claims data must move with them when they switch health plans so providers have access to a complete medical history.
- Reduce redundant procedures and costs: Real-time access to prior claims, medications and lab results helps avoid unnecessary testing and duplicate treatments.
- Empower patients with data access and transparency: Patients gain control over their health information through API-enabled sharing that supports consumer health apps and third-party services.
All CMS-regulated payers, including Medicare Advantage, Medicaid, CHIP and Qualified Health Plans on the Federally Facilitated Exchanges, must comply with this rule. The regulation represents a critical step toward a connected, interoperable healthcare ecosystem where information flows securely, improving care outcomes and efficiency.
Payer Interoperability Challenges
Most health plans and payers face significant challenges as they work to comply with the CMS Payer-to-Payer API Exchange mandate. Meeting the new FHIR-based interoperability requirements demands both technical and organizational readiness. (See CMS-0057-F compliance solutions.)
Legacy Systems: Most payer data platforms were built for batch EDI transactions rather than real-time API communication. These legacy environments make it difficult to support FHIR API integration and cloud-based workflows.
Fragmented Data Sources: Claims, encounter and clinical data often reside in separate systems that use different standards such as X12, HL7 or proprietary formats. This fragmentation prevents a single view of the member’s data and complicates payer data exchange across systems.
Complex Data Transformation: Translating between FHIR, HL7, CDA and X12 requires advanced mapping, validation and normalization. Manual transformations are slow, expensive and prone to error, thus delaying compliance with CMS interoperability rules.
Limited FHIR Expertise: There is a shortage of developers who understand both traditional EDI transactions and modern FHIR implementation guides. This lack of expertise increases project timelines and costs for health plans.
Security and Consent Management: Ensuring secure authorization, data encryption and consent tracking is complex when multiple APIs and third-party systems are involved. Protecting member privacy while maintaining regulatory compliance adds additional risk.
Without a unified integration strategy, payers face higher implementation costs, project delays and the risk of missing CMS compliance deadlines. Successful payer interoperability requires a scalable, standards-based solution that bridges legacy systems with modern FHIR API infrastructure.
The True Cost of Non-Compliance
Non-compliance with the CMS Payer-to-Payer API mandate has tangible operational, regulatory and reputational impacts:
- Regulatory Penalties: Failure to comply risks exclusion from CMS programs or audit findings.
- Member Dissatisfaction: Inability to transfer complete medical histories can lead to poor care experiences and member churn.
- Operational Overhead: Manual data exchange increases cost and complexity.
- Lost Competitive Edge: Payers who enable seamless API-driven data sharing are better positioned to attract members and partners.
Interoperability is not just about compliance; it’s about maintaining continuity of care and strengthening member trust.
How PilotFish Helps Payers Enable Payer-to-Payer API Exchange
PilotFish offers an end-to-end interoperability solution that helps payers rapidly achieve CMS compliance and create scalable, future-ready API infrastructures.
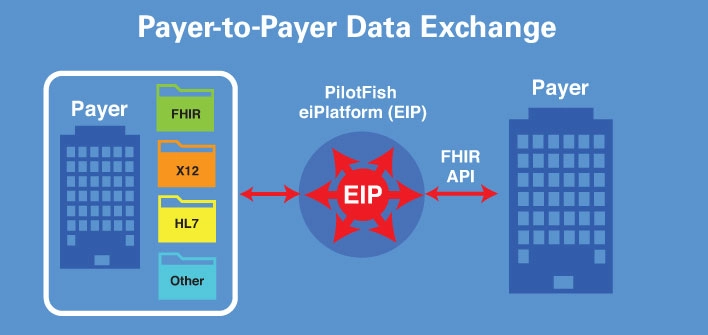
PilotFish eiPlatform (EIP) converts X12, HL7 and other formats to FHIR APIs to enable secure payer-to-payer data exchange
1. Standards-Based, Cross-Protocol Integration
PilotFish natively supports all major healthcare data standards and formats:
- FHIR for payer-to-payer and patient access APIs
- X12 for claims and eligibility transactions
- HL7 v2/v3, CDA, and CCDA for clinical and encounter data
- JSON, XML and flat files for custom or legacy systems
This comprehensive standard support allows seamless data transformation and exchange across any system or partner network.
2. Visual No-Code Interface Assembly Line
The eiConsole enables payers to design integrations visually using a seven-stage Assembly Line.
- Drag & drop mapping between FHIR and legacy standards
- Test and validate in real time within the console
- Reuse and version integrations to accelerate future projects
This approach cuts development time dramatically and eliminates reliance on hard-coded interfaces.
3. Automated FHIR Data Transformation
PilotFish’s FHIR Interface Engine automates the conversion of X12, HL7 or custom data to FHIR resources for API publication. Payers can transform and publish complete member data sets via secure RESTful APIs, ensuring compliance with minimal disruption to existing workflows.
4. Real-Time Monitoring and Compliance Visibility
The eiDashboard provides:
- End-to-end monitoring of all transactions
- Error alerts, message reprocessing and validation
- Audit trails for CMS reporting
Non-technical users can easily oversee message flow and confirm compliance.
5. Secure, Scalable, and Cloud-Ready Architecture
PilotFish supports deployment on-premises, in the cloud or hybrid and integrates with leading platforms like AWS, Azure and GCP. With built-in encryption, access controls and support for containerized (Docker) deployment, payers can scale quickly while maintaining CMS security standards.
Proven Results Across the Healthcare Ecosystem
PilotFish has helped health plans, HIEs and state agencies meet interoperability mandates faster and with fewer resources:
- Health plans modernize EDI and FHIR APIs for seamless payer-to-payer data exchange.
- State Medicaid agencies use PilotFish for CMS data reporting and compliance.
- HIEs integrate multiple payer and provider systems for unified data exchange.
PilotFish’s proven track record of interoperability makes it a trusted partner for payer modernization.
Case Studies That Back Up the Proof
Scaleable Medicaid Data Integration – Statewide CMS compliance through unified data exchange.
Healthcare Data Integration – Automated FHIR mapping from legacy systems.
COVID-19 Reporting Integration – Real-time data exchange for CMS reporting.
FAQs
PilotFish transforms and routes data between payer systems using FHIR APIs and existing formats such as X12 and HL7, ensuring seamless CMS-compliant data exchange.
Yes. PilotFish integrates with identity and consent management systems to ensure secure, member-authorized data transfer.
Absolutely. PilotFish bridges FHIR APIs with legacy X12 transactions, supporting incremental modernization. Watch FHIR to X12 278 video.
Yes. PilotFish supports multi-tenant, cloud-hosted architectures ideal for payers managing multiple lines of business. See Payer integration solutions.
Many payers achieve compliance in weeks, not months, using PilotFish’s visual configuration tools and reusable integration templates.
Check out our FAQ pages for more.
Start Your Payer-to-Payer API Integration Journey
PilotFish simplifies CMS compliance and enables true interoperability among payers, improving member outcomes and operational efficiency.
Let’s build your interoperability roadmap today.
If you’re curious about the software features, free trial, or even a demo – we’re ready to answer any and all questions. Please call us at 813 864 8662 or click the button.
X12, chartered by the American National Standards Institute for more than 35 years, develops and maintains EDI standards and XML schemas.
