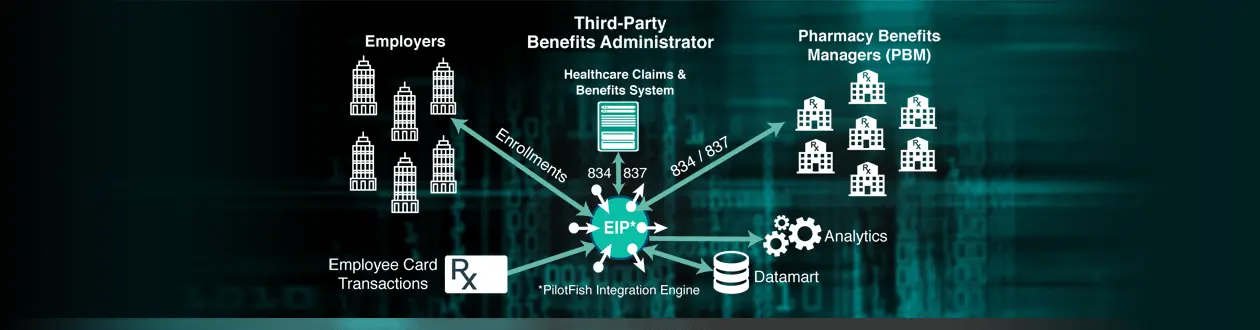
Benefits Administrator Scales EDI 834 and EDI 837 Processing with PilotFish
This full-service third-party benefits administrator (TPA) is a leader in the self-funded employer benefit health and wellness plan space. The company provides employers with strategic benefits plan design, cost-effective benefits administration as well as reporting and analytic services. With PilotFish as a partner, they have been able to capitalize on plan, utilization and claims data to help their customers balance as well as control the costs of providing benefits. In this case study, discover how PilotFish’s Integration Engine solution and deep expertise in EDI healthcare data exchange helped them modernize their IT capabilities and reduce costs.
THE CLIENT
This benefits administrator offers a diverse portfolio of processing, analytics and consulting services. The company prides itself on its best-in-class benefits administration. It manages enrollment, claim processing, premium collection, COBRA notifications, utilization reporting and more for its customers – large employers. To meet aggressive competition, the company is developing a higher level of customization and flexibility to serve its demanding employer customer base. As a trusted partner, PilotFish plays a critical role in helping them develop modernized and responsive IT capabilities.
THE CHALLENGE
The company is tasked with delivering accurate and timely claims processing. It must deal with a wide array of technology issues around egregious billing, repricing, out-of-network providers and variation in accumulator workflows. One-off solutions and manual processes were neither a sustainable model nor ones that would support the client’s high growth trajectory. Costs were too high and response times just too slow.
The company utilizes a third-party system for processing claims, determining eligibility and interfacing with payers. PilotFish was selected by this benefits administrator as the interface engine between client data from multiple sources and their internal third-party payer system. This system is also used to interface with the company’s employer clients.
Never-ending daily challenges arose from having to onboard new employer customers, while also servicing ongoing accounts. Employers reviewed and often switched plan designs and networks on a yearly basis, which added bursts of cyclical work. Employee enrollment periods also added additional pressure and workloads on the IT teams. All these workflows had to be managed while still delivering superior customer service and the high customer satisfaction that a highly competitive market demands.
For this project, there were two primary subsets of interfaces – EDI 834 and EDI 837 inbound and outbound accumulators. In addition to inherent issues of X12 EDI healthcare data, as usual, every customer presented its own set of complexities of inbound and outbound data, data quality to be accommodated and more.
Inbound EDI 837 healthcare claims transactions are ingested into the PilotFish’s eiPlatform where transformations are performed. These are then loaded into their third-party system so that they can be processed with payers. On the outbound side, the process is reversed. The resultant payer EDI files are pulled out of the third-party system, generated into reports and then sent back to the client.
With a large and growing client base, volumes of EDI data arrived daily in widely different quality and formats (EDI, CSV, PDFs, Excel, etc.). Phased automation of X12 EDI transactions such as 834 and 837 (plus NCPDP for client interfacing), was ongoing. Eliminating manual processes and the inefficiencies of legacy systems was the task at hand.
THE SOLUTION
PilotFish, Inc., a leader in healthcare integration, won engagement by this benefits administrator. PilotFish’s integration solution was selected to address the complexity and issues inherent in X12 EDI data integration. A key selection factor for this investment, one that would ensure their long-term growth, is that PilotFish supports every major healthcare standard and source – EDI, NCPDP, HL7, CDA, FHIR, XML and data sources outside of healthcare. It is also fully extensible to support virtually any new standard – no matter how the company’s business evolves.
PilotFish’s eiConsole’s automated graphical interface assembly line process and the visual drag & drop Data Mapper require no custom coding or scripting. Early in the engagement, PilotFish easily dealt with EDI 834, EDI 837 and NCPDP hurdles to ensure data quality and speedier data exchange. Every configuration followed PilotFish’s intuitive user interface and consistent methodology. This ensured that reusability could be leveraged and this capability was built into the process.
PilotFish’s eiConsole for EDI X12 delivers impressive built-in capabilities for incoming data translation, outgoing transaction construction, acknowledgment generation, process orchestration and scheduling.
PilotFish became increasingly relied upon to optimize financial resources and the client’s lean technical team. New priorities and requirements emerged constantly that PilotFish’s nimble team adjusted to.
In one such example, PilotFish was tasked to provide a custom solution to meet the client’s urgent request for an external aid at the front end to organize, schedule and maintain its hundreds of client feeds and requirements.
PilotFish software engineers quickly created an elegant database solution and structured queries to function as the client’s single source of client feed data. Client specifics, job scheduling and routing information are automatically triggered from this optional and separate custom database and used to configure and initialize PilotFish’s Listeners (connectivity protocol adaptors).
Tested in action and acclaimed by the users, the custom database was designed to be easily managed and maintained as part of the responsibilities of a single analyst. The client saw immediate time and money savings.
At every shift in need, priorities or scope – PilotFish was able to rapidly prototype solutions. The impressed IT management has leveraged PilotFish’s software over an ever-greater number of time-critical deliverables. PilotFish’s lead engineers have become valued team members who are relied on for their expertise, innovative solutions and ability to “roll with the punches.”
THE BENEFITS
With PilotFish, only one integration solution was needed across the entire customer base – no matter the data sources or targets. The company’s staff only needed to learn one tool and could leverage PilotFish’s agility in working with databases and data repositories. PilotFish incorporates deep expertise and experience in data exchange and data mapping to seamlessly ensure data quality and reliability. PilotFish’s Integration Engine solution automates and streamlines the integration and interoperability that is the foundation of the company’s benefit-administration and analytic services.
Interfacing with employer systems, third-party vendors, internal databases and employee-facing portals was no problem. Time-consuming manual interventions have become a rarity. One-off solutions ended and became a thing of the past. The company leverages PilotFish’s Data Mapper for extensive and rapid reuse of formats as it experiences rapid growth of its client base. The time and money saving here alone produces impressive ROI.
PilotFish was able to work with the company in a way that worked best for their objectives. Company staff that was available was trained on PilotFish software. That team was augmented with PilotFish software engineers to help them meet critical customer deliverable deadlines. PilotFish enabled the rapid integration of scores of data feeds from an external, automated custom solution. A PilotFish advisor was on hand day-to-day to field support questions and to troubleshoot. When and where it made sense, PilotFish led and implemented the integrations. PilotFish’s problem-solving and innovative solutions significantly helped drive modernization and automation forward – at the pace demanded by executives and growth imperatives.
THE FUTURE STATE
A PilotFish lead software engineer collaborates on an ongoing basis with the company’s IT team to develop and architect technical strategies as well as implement solutions as the need arises. The company has unique advantages as a trusted steward of claims data. Their plan is to leverage their customers’ repositories of integrated data. With PilotFish’s help, the client is on the critical path to offer employers new reporting and comprehensive views into the performance and costs of their health and wellness plans.
New capabilities around EDI 837 repricing are on the roadmap for PilotFish. First order is to eliminate manual intervention and associated costs. Faster, better and more responsive turnaround will contribute to greater customer satisfaction on a thorny issue.
PilotFish has anticipated that client requirements will continue to evolve. It’s why it has architected its solution to be infinitely extensible and flexible. Success after success is why PilotFish’s multi-faceted role continues to evolve and grow at this leading benefits administrator, as it builds new products and delivers competitive advantages.
Since 2001, PilotFish’s sophisticated architecture and innovations have radically simplified how healthcare integration gets done. Today PilotFish offers the most flexibility and broadest support for healthcare integration of any product on the market and is system, platform and database agnostic. PilotFish’s healthcare integration suite includes support for all healthcare data formats (HL7 2.x, HL7 3.x, FHIR, CCD/CCDA, JSON, XML, X12 EDI, NCPDP, etc.) and communication protocols.
PilotFish is architected to be infinitely extensible with our Open API and flexible to meet any integration requirement. PilotFish distributes Product Licenses and delivers services directly to end users, solution providers and Value-Added Resellers. To learn more, visit our Case Studies or specific solutions like HL7 Integration or X12 EDI Integration.
PilotFish Healthcare Integration will reduce your upfront investment, deliver more value and generate a higher ROI. Give us a call at 813 864 8662 or click the button.
HL7 is the registered trademark of Health Level Seven International.
X12, chartered by the American National Standards Institute for more than 35 years, develops and maintains EDI standards and XML schemas.