EDI Claims Processing for Healthcare Providers and Health Payers with PilotFish
Processing and working with EDI claims poses many challenges for Healthcare Providers and Health Payers. X12 EDI has a complex data structure and each EDI message, such as healthcare claim, contains intricate data structures with numerous data elements and codes. The EDI 837 transaction set can include hundreds of data elements. ICD-10 diagnosis and procedure codes consist of tens of thousands of individual codes and descriptors. Healthcare claims processing typically involves hundreds to thousands of data elements and codes.
Mapping these data structures to the appropriate EDI format (such as X12) can be complex and time-consuming. Mapping requires the careful handling of data elements, segments, and loops. Inconsistent or incorrect mapping can lead to data errors or rejection of claims. Another challenge is validating the accuracy, completeness, and consistency of claims data required for successful processing. Payers must comply with industry standards such as HIPAA, X12, or other regional regulatory frameworks. The right EDI solution is essential for achieving efficiency, accuracy, and compliance in your claims management or health claims processes.
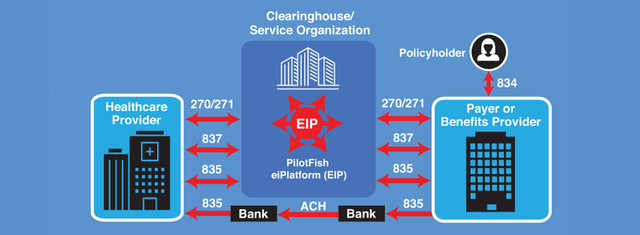
EDI Workflow Example of Clearinghouse Utilizing PilotFish Integration Platform
PilotFish eiSuite – The Best-in-Class X12 EDI Integration Platform
PilotFish offers the best-in-class EDI integration platform designed specifically for the healthcare sector. With our robust EDI solution, you can achieve unparalleled efficiency, accuracy, and compliance.
Our robust data transformation and mapping tools seamlessly convert your internal claims data to the required EDI format, facilitating accurate and compliant data exchange. With PilotFish, you can handle EDI message complexities, eliminating worries over complex mapping challenges and data errors often leading to claim rejections or delays.
With PilotFish, you can effortlessly handle the complexities of healthcare claims, including intricate data structures, hundreds of data elements, and thousands of codes. Our EDI data integration platform provides comprehensive validation, error handling, and compliance with industry standards like HIPAA, upholding the integrity and security of your claims data.
Experience streamlined workflows with real-time processing and automation, thus reducing manual effort and accelerating your claims management. PilotFish also supports seamless connectivity and communication with healthcare providers and intermediaries, enabling smooth EDI message data exchanges and timely claims adjudication.
Gain valuable insights into your claim’s operations through PilotFish’s advanced reporting and analytics features. Track key performance indicators, identify trends, and make data-driven decisions to improve your business processes continuously.
Join leading healthcare organizations that trust PilotFish’s EDI integration platform to optimize their claims management and health claims processes. Make PilotFish your data integration platform and experience a new level of efficiency, accuracy, and compliance.
The PilotFish eiSuite provides a comprehensive solution for claims processing, including claims scrubbing. The eiSuite consists of 4 complimentary offerings:
- eiPlatform – the Java runtime component for unattended execution of your interfaces
- eiConsole for X12 EDI – the IDE and the developer’s workstation for configuring, managing, and maintaining interfaces.
- eiDashboard – a web-based application for interface monitoring and reporting eiSuite
- EDI SNIP4+ – a complete solution suite for X12 EDI integration that supports all X12 transactions, SNIP 1-7 with validation and an optional add-on Code Set Maintenance subscription for updating and maintaining external code sets.
X12 EDI HIPAA Integration
Now let’s look in detail at the features and capabilities offered in the PilotFish eiSuite that streamline data exchange and automate claims handling, including claims scrubbing.
EDI Standard Support & Compliance
In the realm of healthcare claims management and processing, PilotFish distinguishes itself with its comprehensive integration platform. Offering extensive support for various data formats and standards, particularly the widely adopted X12 standard, PilotFish enables healthcare organizations to efficiently process and transform claims-related data while ensuring adherence to industry standards. With its advanced compliance validation capabilities, PilotFish guarantees thorough validation of incoming claims or enrollment data, maintaining compliance with X12 standards and regulatory requirements, thus ensuring that healthcare organizations’ claims management processes are aligned with industry standards and regulations.
- X12 Standards Support: PilotFish extends robust support for diverse data formats and standards, prominently including X12. The integration platform is equipped with capabilities to parse, validate, and generate X12 messages such as EDI 837 (healthcare claims), EDI 834 (benefit enrollment), EDI 835 (healthcare claim payment/remittance advice), and EDI 270/EDI 271 (healthcare eligibility/benefit inquiry and response). This functionality enables seamless processing and transformation of claims-related data in accordance with industry standards.
- Compliance Validation: PilotFish delivers comprehensive validation features to ensure compliance with X12 standards and regulatory mandates. The solution incorporates predefined validation rule sets tailored to X12 transaction sets, facilitating healthcare organizations in validating incoming claims or enrollment data for accuracy, completeness, and adherence to regulatory guidelines.
EDI Data Mapping & Transformation
- Flexible Data Mapping: PilotFish’s user-friendly interface enables healthcare organizations to establish and manage complex data mapping rules, transforming and mapping data elements between internal formats and the X12 EDI format. The 3-pane data mapper allows users to visually align source data elements with their corresponding target X12 elements, specifying necessary transformations, conversions, or value lookups.
- Support for Code Sets and Terminologies: PilotFish’s Data Mapper facilitates the mapping and translation of various code sets and terminologies crucial in healthcare claims processing, including transitioning between proprietary code sets and standard code sets like ICD-10, CPT codes, and HCPCS codes. This ensures seamless conversion and mapping to comply with X12 standards and accurate claims processing.
- Data Validation and Error Handling: Within its data transformation and mapping functionalities, PilotFish incorporates validation and error handling capabilities, enabling healthcare organizations to establish validation rules and data consistency checks. This ensures that the transformed data adheres to required standards and business rules, with any errors or inconsistencies being promptly addressed through built-in error handling mechanisms.
EDI Connectivity & Automation
PilotFish presents significant advantages in claims processing for healthcare organizations with its array of connectivity options and automation capabilities. The platform facilitates effortless connection with healthcare providers, payers, and intermediaries through various protocols, automating workflows for efficient claims management. With proactive error handling and real-time notifications, PilotFish ensures swift issue resolution, promoting streamlined operations, enhanced productivity, and error-free claims processing.
- Broad Connectivity Options: Supporting a wide range of connectivity options, including secure file transfer protocols (FTPS, SFTP), web services (SOAP, REST), and direct integration via APIs, PilotFish enables seamless interaction with various healthcare entities for the exchange of EDI transactions related to claims management. (40+ Listeners)
- Workflow Automation: Through its workflow automation features, PilotFish streamlines the claims management process, incorporating automated routing, event triggers, and exception handling to facilitate efficient claims processing, status tracking, and escalation.
EDI Reporting, Compliance, and Scalability
PilotFish equips healthcare organizations with competitive advantages in reporting, compliance, and scalability for their claims management needs. The platform’s robust reporting and analytics tools provide insights into claims management operations, allowing monitoring of key performance indicators, tracking of claim volumes, and informed decision-making for process enhancements.
- Reporting and Analytics: PilotFish offers reporting and analytics capabilities, providing insurers or payers valuable insights into their claims management operations. The solution offers customizable dashboards and reporting tools, enabling users to monitor key performance indicators (KPIs), track claim volumes, identify trends and make data-driven decisions for process improvement.
- Compliance and Security: PilotFish prioritizes compliance with industry standards, including data security and privacy regulations like HIPAA. PilotFish’s integration solution supports encryption protocols, secure data transmission and access controls to protect sensitive healthcare information during EDI integration. It also supports audit trails to maintain compliance with regulatory requirements.
- Scalability and Integration: PilotFish provides scalability and flexibility to accommodate growing data volumes and integration needs. It supports seamless integration with other internal systems, such as claims management or adjudication systems, enabling insurers or payers to achieve end-to-end automation and optimize the claims management process.
EDI Healthcare External Code Set Maintenance
PilotFish offers a service for the ongoing update and maintenance of the extensive array of X12 EDI codes, which includes sophisticated procedures such as claim auditing and claim scrubbing. With the potential for codes to be updated on varying schedules, PilotFish’s optional subscription service for continuous updates of EDI Healthcare External Code Sets alleviates the burden from customers, integrating essential components like claim scrubbing and claim auditing seamlessly into the EDI SNIP Validation Processor within the eiConsole.
PilotFish – The Proven EDI Integration Platform for Your Success
PilotFish software is utilized by leading healthcare organizations. Its proven EDI claims processing solutions address the challenges associated with complex data structures, data mapping, validation, compliance, and scalability. With a comprehensive suite of features and capabilities, PilotFish empowers healthcare providers and payers to achieve efficiency, accuracy, and compliance in their claims management or health claims processes.
The PilotFish solution supports X12 standards, provides robust data mapping and transformation tools, facilitates seamless connectivity and automation, offers powerful reporting and analytics capabilities, prioritizes compliance and security, and ensures scalability and integration. Additionally, PilotFish’s optional code maintenance service relieves customers of the burden of code updates, ensuring continuous compliance with changing industry requirements. Choose PilotFish for unparalleled performance and success in your healthcare claims management operations.
If you’re curious about the software features, free trial, or even a demo – we’re ready to answer any and all questions. Please call 813 864 8662 or click the button.
HL7 is the registered trademark of Health Level Seven International.
X12, chartered by the American National Standards Institute for more than 35 years, develops and maintains EDI standards and XML schemas.

